Hoboken, Jersey City, Hudson County, and the globe are deep in the trenches in the fight against COVID-19. We’re all in this fight together, but it’s those who are working right there on the frontlines that deserve a real round of applause. Every day, our healthcare heroes and first responders are putting their health + lives at risk to benefit ours.
In an effort to show them some extra gratitude, love, and appreciation, we’ve started a new series to feature and highlight the amazing and dedicated people who are right there on the frontlines. Each time, we’ll share their stories and a way that you can help each individual + his or her team. Additionally, with their permission, we’ll be sharing their respective Venmo accounts, if you would like to spread some joy to them with a direct donation {think buying them a meal, a coffee, or just a little pick-me-up to show your appreciation}.
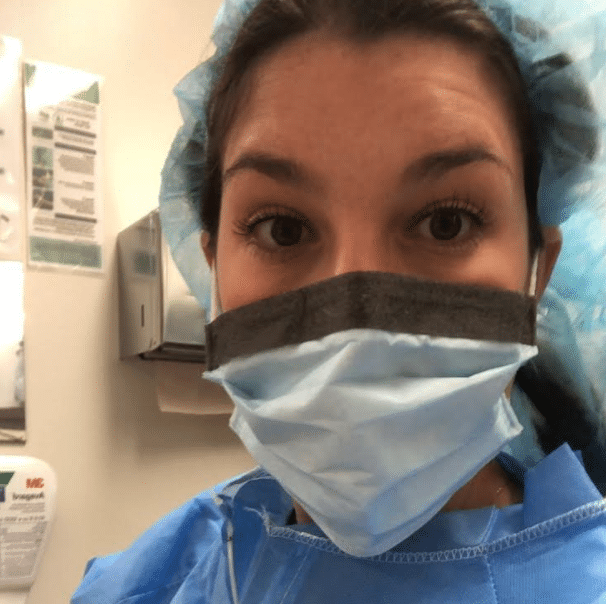
This time around, we spoke with Alexandra Grippo, a Jersey City-based ICU nurse working at New York-Presbyterian in NYC. Keep reading for her story, and how you can help Alexandra and her hospital unit at NYP directly.
Have a health care provider you want to submit for a feature? Email their contact info to hello@hobokengirl.com!
PS: Make sure to go to your windows/balconies nightly to cheer all of our incredible healthcare professionals at 7:00PM each evening.

Tell us about yourself.
My name is Allie, I moved to Jersey City this past October. I lived in the city for four years and wanted more space {mostly because I wanted a dog} and a change of pace.
What is your current occupation and how long have you worked there?
I’m a nurse at New York-Presbyterian, I’ve worked there for four and a half years.
What was your original career plan? How did you get into this career?
I always knew I wanted to be a nurse. As clichés as it sounds, I knew I needed to pursue a career that I would be making a difference. I have way too much energy to sit at a desk anyway!
See More: Sean Healey, Patient Care Tech at Holy Name Medical Center
What has been the hardest day/scariest day on the job?
The scariest days are now. Everyone is on high alert; we don’t know what is going to happen minute by minute to our patients. The last shift I worked with three patients who were decompensating simultaneously. We had to split nurses and doctors to those three patients while other nurses kept an eye on the rest of the unit. Two of those patients we decided to paralyze, for a total of four on the unit.
Paralyzing a patient is the last resort when sedation and pain medications aren’t enough and they are still fighting the ventilator. When a patient is fighting the ventilator, we call it being desynchronized with the vent, it occurs for several reasons but we need to act quickly to ensure the patient’s demands are being met. Paralyzing a patient allows us to fully control their breathing with the ventilator. That was just a few minutes of the shift that left us exhausted and scared. We are scared of what will happen if we have to code a patient, every time an alarm goes off on the cardiac monitor or vent it causes physical reactions that we won’t be able to get PPE on quick enough to save the patient. Each shift, each minute our minds are racing on what to do next because during COVID there are no breaks.
Who is someone you look up to/your hero?
My hero is my mom. She passed away from cancer in November 2018, but she is the sole person that gets me through all the challenges at work, especially now. She was by far the strongest, most caring, genuine, woman I will ever know and my biggest supporter.
So far, what has been the highlight of your career?
The highlight of my career by far is becoming an ICU nurse. This was my last big accomplishment before my mom passed. She was so proud of me, telling all her friends, and of course, made a cheesy FB post to brag about me. Little did I know when I accepted the job that my co-workers would have such a positive impact on my life.
I can say without a shed of doubt the nurses and doctors I work with are the hardest working and caring individuals. The nurses I work with truly care about their jobs and every patient we take care of. We are dedicated to our unit and making it the best place for our patients and coworkers, we are constantly brainstorming and launching new projects and policies to ensure we are providing the best care. These nurses saved me by getting me through the darkest days of my life after my mom passed and I am forever grateful for them.
What qualities does a person need to do your job?
To be a nurse in the ICU you need to be adaptable, strong-willed, caring, a team player, and definitely have a sense of humor. You need to want to be a nurse. Being a nurse is mentally and physically exhausting at times but when we hear from patients or their families after they’ve left the ICU that they are doing well, makes it all worth it.
What’s something that people wouldn’t expect about what you do on a daily basis?
Titrate life-sustaining IV drips without doctors telling us to do so. So many patients’ families ask, “doesn’t the doctor have to do that?” Nope! Once the order for the medication order is on the computer, we titrate based on our nursing judgment.
Describe a typical day on the job.
We don’t really have a typical day; working in an ICU, each shift brings its own challenges and you never know what to expect. Generally, we start each shift getting a report from the previous nurse. Then we do a full head-toe assessment, check all the IV pumps to make sure they are programmed correctly, calibrate/zero any machines in the room, and look at the ventilator to see how the patient is breathing. We collaborate with respiratory therapists and residents throughout the shift to manage our patients. As ICU nurses, we take our patients to MRI/CT scan with a respiratory therapist if the patient is on the ventilator. At night we bath patients every shift to prevent infections. During every admission in the ICU, there are at least three nurses in the room, the primary nurse gets the report, one nurse will document, and the other will start connecting the patient to our monitor. Each patient is so different and you really never know what is going to happen each time you walk onto the unit.

How do you spend your free time?
Aside from spending time with friends and family, I love being with my new pup, Blue! I rescued her from the Joy Rides Rescue, an amazing local rescue! Blue has been my bright spot during this uncertain time. I also love reading and listening to every crime podcast!
Are there organizations that you feel strongly about and support? Tell us about them.
I am involved with LUNGevity, the nation’s leading lung cancer-focused nonprofit. When my mom was diagnosed with lung cancer in 2016, I knew I needed to use my voice to spread awareness that anyone who has lungs can get lung cancer. The first event I participated in through LUNGevity was their Breathe Deep walk in NYC on October 27th, 2018. Being involved in the walk, even though my mom was not able to be there, gave me the opportunity to make her proud one last time. My mom lost her battle to cancer in November 2018, and I will continue to be involved in LUNGevity in her memory to spread awareness, hope, and education.
What has been the biggest challenge you’ve faced as a healthcare worker during this pandemic?
The unknown. This virus is new to everyone across the globe therefore, we don’t know the proper way to handle it, how to treat it, how to adequately prevent the spread, and even the best way to protect ourselves. Each shift at the hospital is something that is changing, there is no constant anymore and that can be scary. Despite everyone’s best efforts, the unknown will continue to be unknown until we are able to conduct more research which may be months to years from now. Also, of course, the quickly dwindling resources. I am lucky right now to work at a hospital that still has proper PPE but we are taking every action to keep it that way, for example reusing masks when possible.
What are the most common symptoms you’re coming across?
Every patient is presenting very similar, fatigue, shortness of breath, fever, and loss of taste/smell.
What is one thing you want the public to know about the virus?
It needs to be taken seriously. As an ICU nurse, my colleagues and I are exposed to blood, bodily fluids, other viruses, feces, urine, but this is a different beast. This beast we don’t know how to treat. This virus isn’t prejudiced, it will infect anyone and everyone, despite age.
Read More: Maxim Casas, ER Nurse at Christ Hospital in Jersey City
Do you know anyone personally affected by the virus?
I do have a few colleagues that have the virus and thankfully are recovering.
How can we help? What can we do?
Stay home, please! Social distancing means stay home! It is so disheartening to see your friends and other people not taking the virus seriously and still going to friends’ houses, interacting with people outside, and being careless. Healthcare workers are going to work every day for the public and it’s really frustrating to see some people’s lack of empathy for what we are doing to for them every single day.
If someone wanted to donate food/supplies/etc to you/your team, how could they do that?
They could Venmo me {@Allie-Grip} or send me a DM {@alliegrip}!
Have a health care provider you want to submit for a feature? Email their contact info to hello@hobokengirl.com!
PS: Make sure to go to your windows/balconies nightly to cheer all of our incredible healthcare professionals at 7:00PM each evening.










